Blog
Find out more on articles related to infectious diseases : Bacteria - virus - fungi.
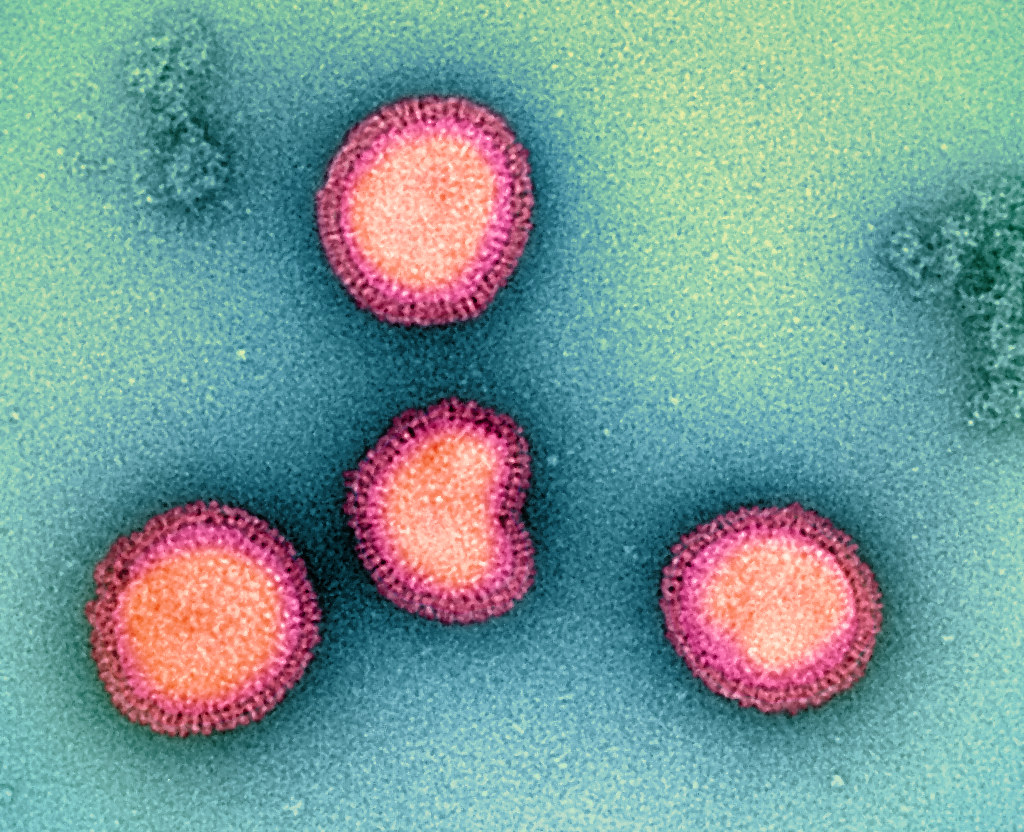
While seasonal flu is often spoken of as a single entity, Influenza B tends to remain in the shadow of its cousin, Influenza A — yet its health and economic burden is far from negligible.
Did you know that Influenza B accounts for nearly one-third of seasonal flu cases each year?
Effective management of AMR and CC demands robust economic and political actions. Global and national plans should be aligned to address these interconnected challenges. Policies need to encourage the responsible use of antimicrobials and foster environmental sustainability.
In the face of escalating antimicrobial resistance (AMR), researchers and innovators are turning to advanced technologies like Artificial Intelligence (AI) and genomic sequencing to pave new roads in the battle against superbugs.
In the wake of the upcoming UN General Assembly, the spotlight turns to a pressing global health challenge: antimicrobial resistance (AMR).
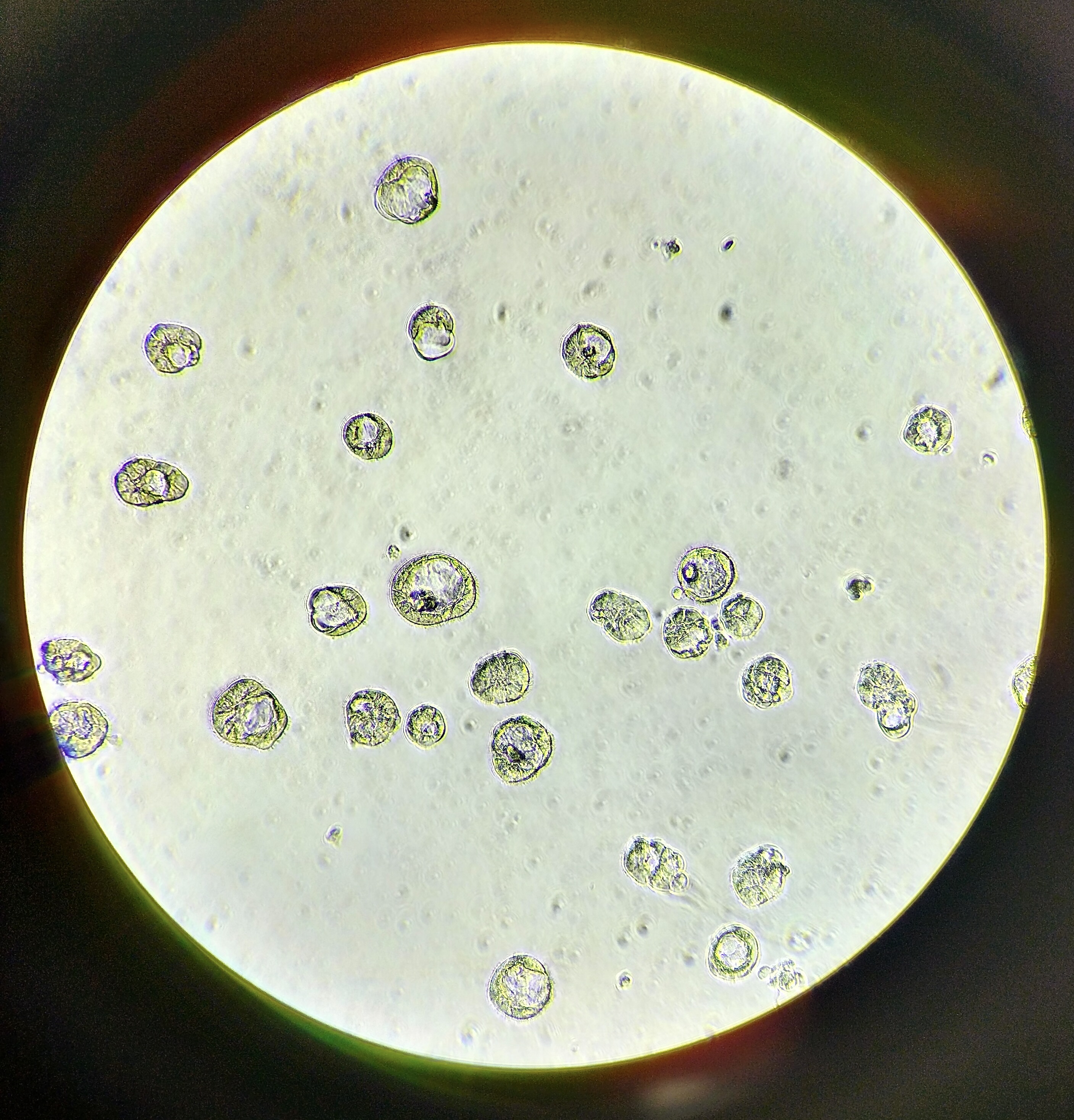
Escherichia coli, commonly referred to as E. coli, is a familiar term to many. It is a rod-shaped bacterium that is typically found in the lower intestines of warm-blooded organisms, including humans.
Bacteria rely on a system called quorum sensing (QS) to sense population density and make collective decisions.
The 6M € granted to IN-ARMOR project will optimize an already developed drug platform using Computer Aided Drug Design.
Vibiosphen’s constant objective is to develop innovative and translational experimental models that would ultimately result in the decrease of the number of animals used for preclinical testings.
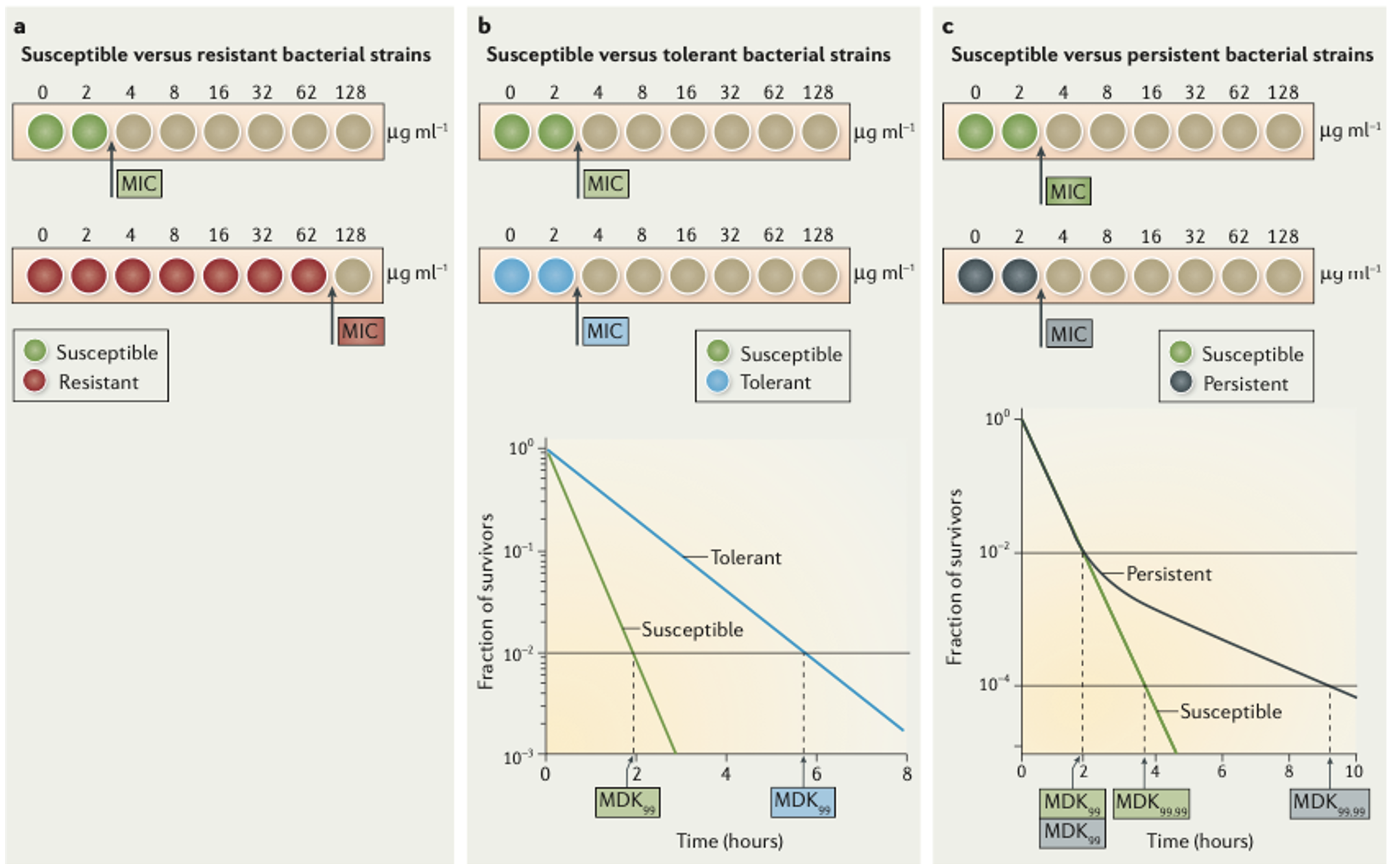
By zooming in the mechanism that bacteria use to escape the antibiotics, we find three different subgroups – resistance – tolerance – persistence.
Distinguishing these three groups is key in the fight against bacterial infection.
A collaboration between 3 players : L’oréal – Qima – Vibiosphen
Our last collaboration led to a great publication to understand the aetiology of dandruff, and specifically the role of Malassezia restricta.
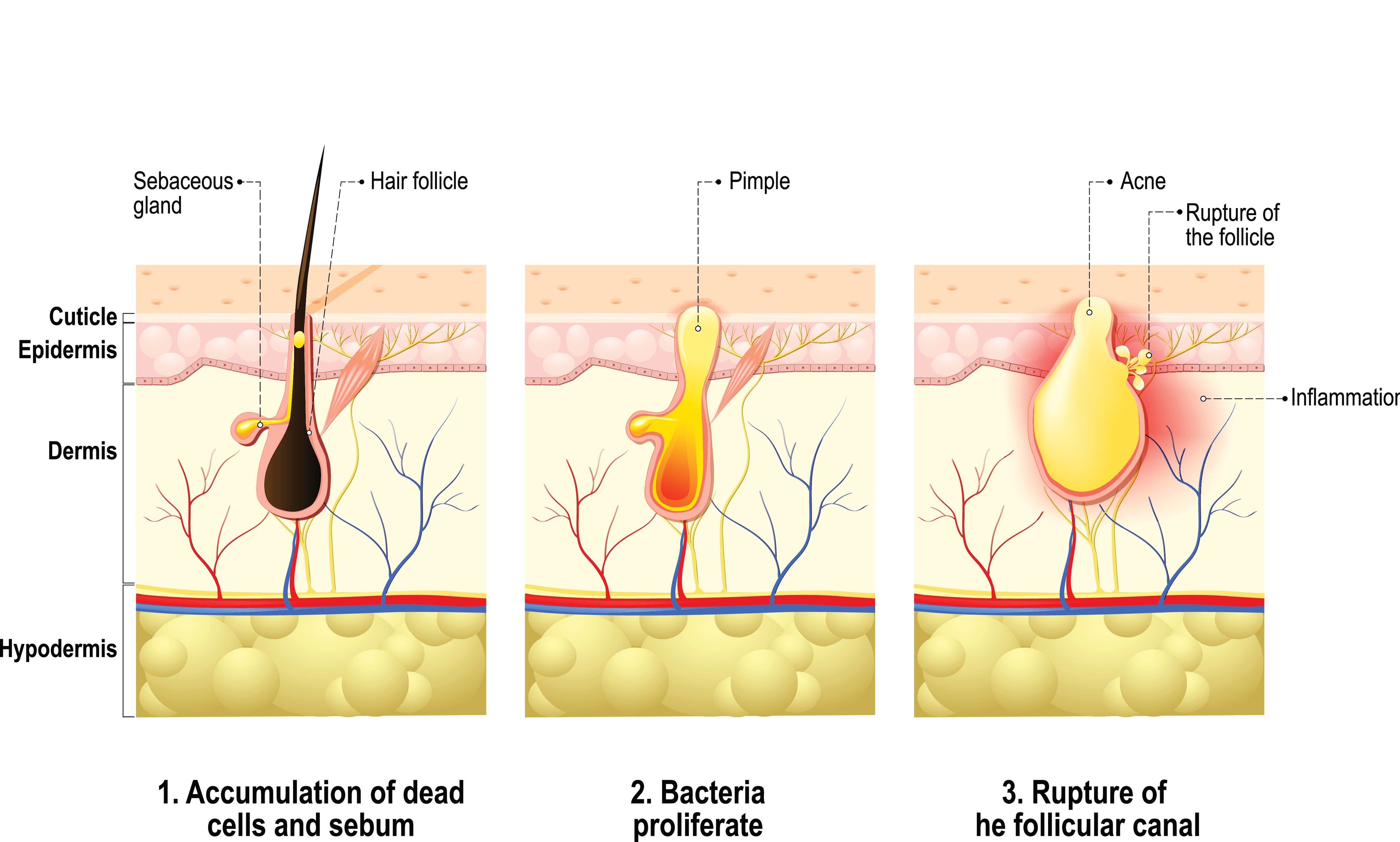
Acne vulgaris is a common inflammatory disorder affecting more than 80% of young adolescents. Cutibacterium acnes plays a role in the pathogenesis of acne lesions, although the mechanisms are poorly understood.
Recent advances in sequencing technology have demonstrated that the development of AD not only associates with the skin microbiome, but also with gut microbiota. In other words, unbalanced gut microbiome or intestinal permeability may lead to a loss of integrity of the skin barrier that might trigger predispositions to atopic dermatitis in this case.
Pagination
Catégories
Pagination
- Page précédente
- Page 2
Archives
- novembre 2021 (1)
- décembre 2021 (2)
- janvier 2022 (3)
- février 2022 (2)
- avril 2022 (1)
- mai 2022 (3)
- juin 2022 (1)
- octobre 2022 (1)
- décembre 2022 (1)
- février 2023 (1)
- avril 2023 (2)
- mai 2023 (1)
- août 2023 (1)
- septembre 2023 (1)
- avril 2024 (2)
- mai 2024 (1)
- mars 2025 (1)
- mai 2025 (1)
- juin 2025 (3)
- juillet 2025 (1)
- octobre 2025 (1)
- janvier 2026 (2)
- février 2026 (2)
- mars 2026 (2)